Robotic-assisted spine surgery
Washington University spinal neurosurgeons are national experts in the use of robotic-assisted minimally invasive spine surgery. They use new, innovative robotic technology to perform spinal fusions. This new technology has been demonstrated to increase patient safety, improve accuracy and reduce patient exposure to radiation.
Robotic-assisted minimally invasive spine surgery uses a navigational system in which a computer merges the CT and X-ray images to map the anatomy and guide neurosurgeons in the procedure including placement of screws.
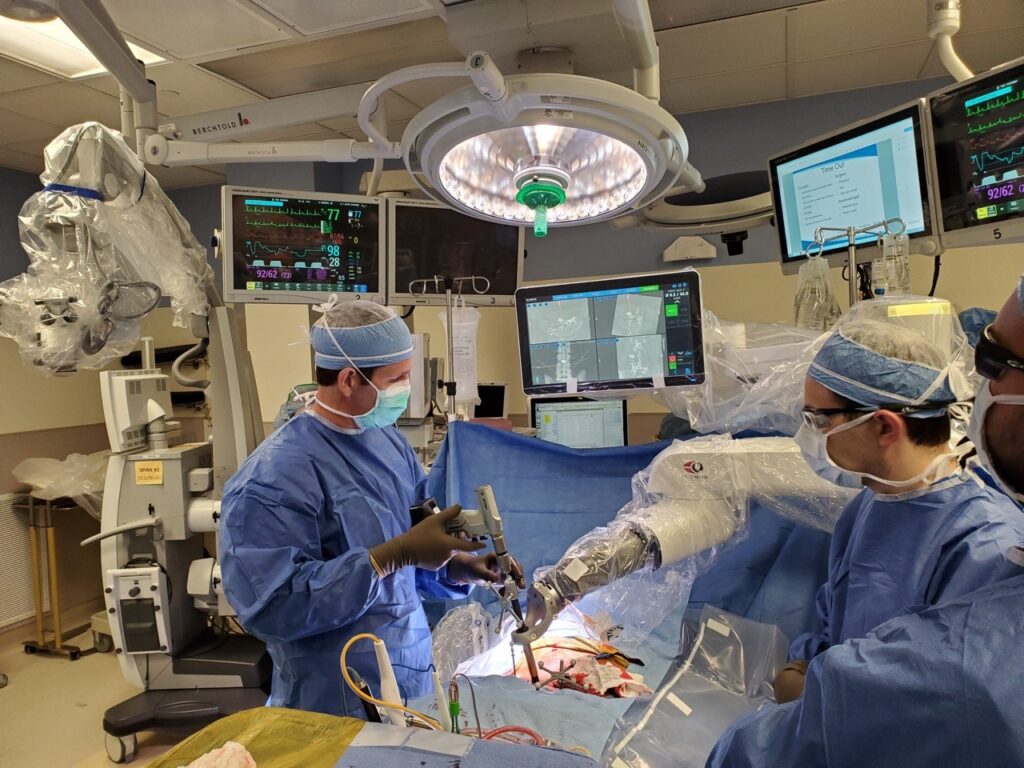
The technique significantly reduces the level of radiation exposure for patients and the operating team and allows the neurosurgeon to better plan incisions and the sophisticated screw placement needed in the operation.
Patients spend several days in the hospital after an open spinal fusion, but less than 24 hours with minimally invasive operations. There is typically less pain, faster recovery, and reduced need for pain medication following minimally invasive procedures.
Washington University neurosurgeons were the first to perform navigated robotic-assisted minimally invasive spine surgery in the State of Missouri.